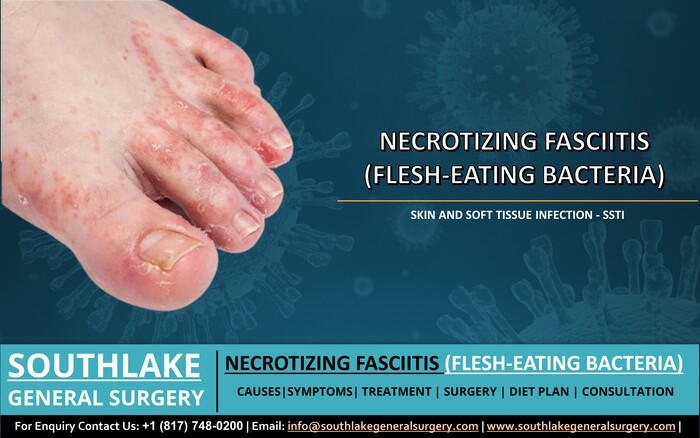
Necrotizing fasciitis, also known as flesh-eating bacteria, is a group of bacteria that cause severe Skin and Soft Tissue Infections (SSTI). The bacteria cause tissue to die, which causes large areas of skin to become discoloured and to become painful, red, and swollen.
What Are Flesh-Eating Bacteria (Necrotizing Fasciitis)?
The bacteria are spread through direct contact with a person or animal who has the infection or through close contact with surfaces and items that are contaminated with the bacteria. The most common causes of necrotizing fasciitis include group A Streptococcus, also known as group A strep, and staphylococcus aureus.
Necrotizing fasciitis is an uncommon infection of the skin and subcutaneous tissues caused by flesh-eating bacteria. Failure to promptly treat this condition can be fatal. When someone is afflicted with necrotizing fasciitis, it spreads rapidly and aggressively.
It is estimated that 500 to 700 new cases are discovered in the United States each year. More than a quarter to a third of those cases end in death. Children are very infrequently affected by this.
What causes flesh-eating bacteria and what puts you at risk?
In most cases, necrotizing fasciitis is caused by bacteria belonging to the group A streptococcus (GAS) family. Strep throat is an infection caused by the same sort of bacteria as this one. However, several bacterial strains, including staphylococcus and others, have been identified as being associated with the condition.
Necrotizing fasciitis is a condition that occurs when certain kinds of bacteria invade the superficial fascia, which is a layer of connective tissue that lies just below the skin.
The spread of flesh-eating bacteria
Necrotizing fasciitis is caused by bacteria that can get into the body in several ways.
- Infected surgical sites
- Injuries such as puncture wounds
- Insect bites
- Minor cuts or abrasions
- Burns
It’s not always clear where an infection came from. If the illness has taken root, it will quickly damage the body’s muscles, skin, and fatty tissue.
If your immune system is compromised and you have certain conditions, you may have an increased risk of contracting flesh-eating bacteria (necrotizing fasciitis). The following medical issues may put you at an increased risk:
- Cancer
- Chickenpox
- Diabetes
- Use of steroids
- Cardiovascular illness that affects the heart valves
- Lung disease
- Cirrhosis
- Alcohol abuse
- Peripheral vascular disease
- Chronic Kidney disease
- The use of intravenous or injectable medications
- Tuberculosis
What are the symptoms of Flesh-Eating Bacteria?
Flesh-eating bacteria infections typically manifest their earliest symptoms within the initial 24 hours after infection. The symptoms can be mistaken for the flu or a milder form of skin infection. Early signs include – fatigue, nausea, inflammation, and pain in the surgical area.
Many times, a combination of the following symptoms occurs:
- Pain that exceeds what one would anticipate based on the superficiality of the wound.
- Worsening discomfort around the site of a minor skin wound.
- Cold and flu-like symptoms, including fever, chills, headache, fatigue, and general malaise.
- Dehydration-induced severe thirst.
- Patches of redness and warmth near the wound, though these symptoms may first appear elsewhere.
Within 3–4 days of infection, more advanced symptoms appear near the painful infection site. They include:
- Blisters that start with a deep violet colour and eventually rupture, leaking a dark, putrid fluid.
- Changes in hue, peeling, and flaking because of tissue death (gangrene)
- There may be swelling and a purple rash.
The following are critical symptoms that often manifest within 4–5 days after infection:
- The effects of a toxic shock
- Significant decrease in blood pressure
- Unconsciousness
How to diagnose Flesh-Eating Bacteria?
Necrotizing fasciitis, which is caused by flesh-eating bacteria, has an immediate impact on the body, and receiving an early diagnosis is critical to the patient’s chance of survival.
Your doctor will do a thorough examination and take a detailed medical history. Doctors will likely admit you to the hospital and conduct tests there if they fear you have flesh-eating bacteria because of the seriousness of the situation.
Some diagnostic procedures for necrotizing fasciitis (flesh-eating bacteria) include:
- Blood tests. A high number of white blood cells are present in people infected with flesh-eating bacteria.
- Tissue Biopsy. It’s possible that exploratory surgery will be required to remove contaminated tissue. Researchers analyze the tissue to determine which bacteria are responsible for the infection. However, antibiotics will be prescribed for you to take before the lab results are available.
- CT scan. The accumulation of pus and fluid can be visualized on a CT scan, allowing the doctor to treat the problem more effectively. Furthermore, it demonstrates subcutaneous gas bubbles, further supporting the diagnosis.
Necrotizing fasciitis is an infection that spreads by close contact, therefore anyone who lives with or has been in close touch with someone who has it should get checked if they develop any symptoms of infection themselves.
How to treat Flesh-Eating Bacteria?
A multifaceted approach will be used to treat patients infected with flesh-eating bacteria. Depending on how far along the illness process you are when treatment begins will determine how far you can expect to get. You are going to get this as a part of the treatment:
- Antibiotics are given intravenously (IV).
- Transfusions of blood are a common medical procedure.
- It’s possible that doctors will suggest you undergo hyperbaric oxygen therapy to protect any healthy tissue.
- Medicines to increase blood pressure.
- Immunoglobulin is infused intravenously. As a result, the body’s natural defenses against infection are bolstered.
- The surgical removal of infected or diseased tissue.
- In severe circumstances, amputation of the damaged limb.
- Breathing aids and heart rate monitors.
What are the complications of Flesh-Eating Bacteria?
Infrequent but potentially life-threatening consequences include:
- Failure of an internal organ
- Amputation-caused limb loss
- Shock
- Death
- Sepsis
- Intense scarring
What is the prevention of Flesh-Eating Bacteria?
One of the most important things you can do to protect yourself from flesh-eating bacteria and other skin illnesses is to practice good hand hygiene by regularly washing your hands with soap and water or you can also use a hand sanitizer that contains alcohol. To avoid skin infections, you should:
- Always use soap and water to disinfect any cuts or open wounds.
- Seek medical attention for any serious or deep wounds, including those caused by punctures or gunshots.
- If you have a wound that is open or a skin infection, you should not use a hot tub or go swimming.
- A clean, dry bandage should be applied over bleeding, draining, or an open wound after it has been cleaned.
The infection caused by flesh-eating bacteria cannot be prevented by a vaccine at this time.
The Prognosis for Flesh-Eating Bacteria
To successfully combat this unusual skin condition, prompt diagnosis and strong therapy are essential. To completely eradicate sick or diseased tissue, many patients require multiple surgeries. Book an appointment with your doctor if your skin is red and puffy for no apparent reason.
Appointment
For more information on Skin and Soft Tissue Infections such as Necrotizing Fasciitis (Flesh-Eating Bacteria), you can contact our healthcare expert today at +1(817) 748-0200.