A small bowel resection is a surgical procedure involving removing a portion of the small intestine. This procedure is typically performed to treat conditions such as bowel obstruction, Crohn’s disease, tumors, or intestinal injuries.
By removing the affected section of the small intestine, small bowel resection aims to alleviate symptoms, restore normal bowel function, and improve the patient’s overall health.
Key Highlights
- A small bowel resection is a surgical procedure involving removing a portion of the small intestine.
- This procedure is specifically designed to address severe gastrointestinal (GI) conditions.
- This procedure is typically performed to treat conditions such as bowel obstruction, Crohn’s disease, tumors, or intestinal injuries.
- By removing the affected section of the small intestine, small bowel resection aims to alleviate symptoms, restore normal bowel function, and improve the patient’s overall health.
- Patients need to be aware of these potential complications and promptly report any concerning symptoms to their healthcare provider for appropriate management.
- Regular follow-up appointments with their healthcare team are crucial for ongoing monitoring and support post-surgery.
Overview of Small Bowel Resection
A small bowel resection is a surgical procedure that is commonly performed to treat various conditions affecting the small intestine. It involves the removal of a portion of the small intestine that is diseased or damaged, allowing for the restoration of normal bowel function.
This procedure is typically recommended when other treatment options, such as medication or dietary changes, have been ineffective in managing the underlying condition. Expert surgeons who specialize in gastrointestinal procedures frequently perform small bowel resections, ensuring the best outcome for the patient. Small bowel resections are typically performed as a last resort.
During the procedure, the surgeon will make an incision in the abdomen to access the small intestine. They will carefully remove the affected section of the small intestine, taking care to preserve the healthy tissue.
After the removal, the surgeon will then connect the remaining sections of the small intestine to ensure the continuity of the digestive tract. This may involve sutures or the use of specialized stapling devices.
Once the procedure is complete, the incision will be closed, and the patient will be closely monitored during the recovery period.
Importance of understanding the procedure
Understanding the procedure is crucial for patients and their families to make informed decisions about their healthcare. It allows them to have realistic expectations about the surgery and its potential outcomes.
Additionally, understanding the procedure can help alleviate anxiety and fear, as patients will have a clear understanding of what to expect during the surgery and recovery process. It also enables patients to actively participate in their care by asking questions, voicing concerns, and following post-operative instructions more effectively.
Overall, having a comprehensive understanding of the procedure promotes better communication between the patient and healthcare providers, leading to a more successful surgical experience and improved patient outcomes.
Who needs a Small Bowel Resection?
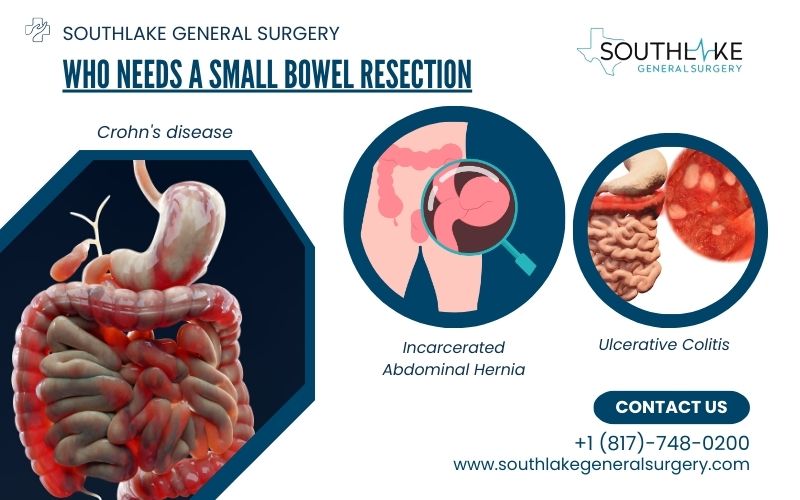
This procedure is specifically designed to address severe gastrointestinal (GI) conditions. Here are some examples: Crohn’s disease, bowel obstruction, perforation, and tumors.
- Incarcerated abdominal hernia, which occurs when a portion of the intestine becomes trapped in the abdominal wall, is another condition that may necessitate a small bowel resection.
- Abnormal growths, such as polyps or cancerous tumors, can also be a reason for a small bowel resection.
- Necrotizing enterocolitis, a serious condition that primarily affects premature infants, can also lead to the need for a small bowel resection. In cases where the small bowel becomes twisted or obstructed, a resection may be necessary to restore normal bowel function and prevent further complications.
- Congenital GI disorders, such as intestinal malrotation or Meckel’s diverticulum, may also require a small bowel resection.
- Chronic inflammatory GI issues, such as ulcerative colitis or diverticulitis, can also be treated with a small bowel resection.
- Trauma or perforation, such as from a gunshot or knife wound, can also necessitate a small bowel resection. In these cases, the injured portion of the small bowel may need to be removed to prevent infection or further damage to the surrounding organs. Prompt surgical intervention is crucial to repair the perforation and prevent life-threatening complications such as peritonitis.
- Small bowel obstruction, often caused by adhesions or tumors, can also be a reason for a small bowel resection. In this condition, the passage of digested food through the small intestine is blocked, leading to severe pain, vomiting, and an inability to have a bowel movement. Surgery is usually required to remove the obstruction and restore the normal flow of digestion.
What are the symptoms and complications that may indicate the need for surgery?
Symptoms and complications that may indicate the need for small bowel resection surgery include:
1. Perforation: If there is a perforation in the small intestine, it can lead to life-threatening complications such as peritonitis. Surgery is necessary to repair the perforation and prevent further complications.
2. Small bowel obstruction: Adhesions or tumors can cause a blockage in the small intestine, leading to symptoms like severe pain, vomiting, and an inability to have a bowel movement. Surgery is typically required to remove the obstruction and restore normal digestion.
3. Inability to pass digested food: If there is a blockage in the small intestine, it can prevent the passage of digested food through the digestive tract. This can result in severe pain, vomiting, and an inability to have a bowel movement. Surgery is usually needed to remove the obstruction and allow for proper digestion.
4. Complications of adhesions or tumors: Adhesions or tumors in the small intestine can lead to complications such as bowel perforation, abscess formation, or intestinal bleeding. These complications may require surgical intervention, including small bowel resection.
5. Unsuccessful non-surgical treatments: In cases where non-surgical treatments such as medication or dietary changes have not been successful in relieving symptoms or resolving complications, surgery may be necessary.
6. Diagnosis of underlying conditions: If an underlying condition such as Crohn’s disease or cancer is diagnosed and causing significant damage to the small intestine, surgery may be recommended as part of the treatment plan.
It is important for patients experiencing these symptoms or complications to consult with a medical professional who can evaluate their condition and determine if small bowel resection surgery is necessary for their case.
What are the diagnostic tests used to determine the need for a small bowel resection?

1. Physical examination: A medical professional may conduct a physical examination to assess the patient’s symptoms, such as abdominal pain, bloating, or changes in bowel movements.
2. Blood tests: Blood tests can help identify any abnormalities that may indicate an underlying condition or inflammation in the small intestine.
3. Imaging tests: Various imaging tests may be used to visualize the small intestine and detect any abnormalities or complications. This may include:
- X-ray: A simple X-ray can provide initial information about the condition of the small intestine.
- CT scan: A computed tomography (CT) scan can provide detailed images of the small intestine and help identify any structural abnormalities or complications.
- MRI: Magnetic resonance imaging (MRI) uses powerful magnets and radio waves to create detailed images of the small intestine.
- Capsule endoscopy: This involves swallowing a pill-sized camera that takes pictures as it travels through the digestive system, allowing for a thorough examination of the small intestine.
4. Endoscopic procedures: These minimally invasive procedures involve inserting a flexible tube with a camera into the digestive tract to evaluate the small intestine. This may include:
- Upper endoscopy (esophagogastroduodenoscopy): This procedure involves inserting a flexible tube through the mouth to examine the upper part of the digestive tract, including the small intestine.
- Colonoscopy: While primarily used to examine the colon, a colonoscopy can also provide information about certain conditions affecting both the large and small intestines.
- Balloon-assisted enteroscopy: This specialized endoscopic procedure allows for visualization and potential intervention within specific parts of the small intestine.
5. Biopsy: In some cases, a tissue sample (biopsy) may be taken during an endoscopic procedure to further investigate any suspicious findings or confirm a diagnosis.
6. Consultation with specialists: Depending on individual cases, medical professionals may consult with other specialists, such as gastroenterologists or surgeons, to determine the need for small bowel resection based on the results of the diagnostic tests.
What are the Preoperative Preparations for a small bowel resection?
Preoperative preparations for a small bowel resection may include:
1. Evaluation: The patient will undergo a thorough evaluation to assess their overall health and determine if they are a suitable candidate for surgery.
2. Medical history: The medical team will review the patient’s medical history, including any previous surgeries, current medications, and known allergies or medical conditions.
3. Laboratory tests: Blood tests may be performed to check for any underlying health conditions or abnormalities that could affect the surgery or recovery process.
4. Imaging studies: Imaging tests such as X-rays, CT scans, or MRI scans may be ordered to obtain detailed images of the small intestine and surrounding structures to help plan the surgical procedure.
5. Bowel preparation: The patient may need to follow specific instructions for bowel preparation, which typically involves taking laxatives or undergoing a bowel cleansing procedure to ensure the intestines are clean before surgery.
6. Medications: The medical team will review the patient’s current medications and advise on which ones should be continued or temporarily stopped before the surgery. This includes discussing blood thinners and antibiotics.
7. Fasting: The patient will typically be instructed not to eat or drink anything for a certain period before surgery, usually starting at midnight on the night before the procedure.
8. Discussion of risks and benefits: The surgeon will have a detailed discussion with the patient about the potential risks and benefits of the small bowel resection procedure, as well as what they can anticipate during and after surgery.
9. Consent forms: The patient will be required to sign consent forms acknowledging that they understand the procedure and its risks and that they agree to proceed with it.
10. Preoperative instructions: The medical team will provide specific instructions regarding when to arrive at the hospital, what to wear, any personal items that should be brought along, and other logistical details related to the day of surgery.
Small Bowel Resection Procedure
During a small bowel resection procedure, the surgeon will remove a portion of the small intestine that is diseased or damaged. This can be done using either a laparoscopic or open approach.
1. Laparoscopic Surgery: In this technique, several small incisions are made in the abdomen. The surgeon will then insert a laparoscope (a thin tube with a camera) and other surgical instruments through these incisions. A laparoscope enables the surgeon to have a clear view of the surgical site through a monitor.
2. Open Surgery: In an open approach, a larger incision is made in the abdomen to access the small intestine directly. This provides the surgeon with more direct visualization and access to the affected area.
3. Preparation: Before surgery, patients will need to follow preoperative instructions provided by the medical team. This may include fasting for a certain period of time before surgery, stopping certain medications, and completing any necessary preoperative tests or evaluations.
4. Anesthesia: Before the procedure begins, anesthesia will be administered to ensure that the patient is comfortable and pain-free during surgery. The type of anesthesia used will depend on various factors, such as patient preference, medical condition, and the surgeon’s recommendation.
5. Incision and exposure: Once anesthesia takes effect, the surgeon will make either several small incisions (laparoscopic approach) or one larger incision (open approach) in the abdomen to gain access to the small intestine.
6. Resection: The diseased or damaged section of the small intestine will be carefully located and removed by either cutting it out (resection) or bypassing it with sutures (anastomosis). The remaining healthy portions of the intestine are then reconnected, if necessary.
7. Closure: After removing or bypassing the affected area, the surgeon will close any incisions made during the procedure using sutures or staples.
Recovery and Postoperative Care

After a small bowel resection, what can I expect?
After a small bowel resection, you can expect the following:
1. Recovery in a monitored area: The patient will be closely monitored in a recovery area until you wake up from anesthesia.
2. Pain management: Pain medication may be prescribed to help manage any discomfort you may experience.
3. Antibiotics: You may be prescribed antibiotics to prevent any infections.
4. Detailed postoperative instructions: The medical team will provide detailed instructions regarding your diet, activity restrictions, wound care, and medication management.
5. Activity restrictions: You may be advised to avoid strenuous activities and heavy lifting for a certain period of time.
6. Wound care: You will need to follow specific instructions on how to care for your incision site.
7. Follow-up appointments: You will likely have follow-up appointments with your surgeon to monitor your progress and address any concerns or complications that may arise.
After a small bowel resection, how much time does one typically need to recover?
Recovery from a small bowel resection can vary depending on individual factors, but it typically takes several weeks to a few months. The medical team will provide detailed instructions on how to aid in your recovery, including diet recommendations, activity restrictions, wound care, and medication management.
It is important to follow these instructions closely and attend follow-up appointments with your surgeon to monitor your progress and address any concerns or complications that may arise during the recovery process.
Potential Complications and Risks
Common complications and risks that may arise after small bowel resection include:
1. Infection: This can occur at the incision site or within the abdominal cavity. It is important to follow proper wound care instructions and take prescribed antibiotics to prevent and treat infections.
2. Bowel obstruction: Scar tissue formation or narrowing of the remaining bowel can lead to a partial or complete blockage, causing symptoms such as severe abdominal pain, bloating, and vomiting. It is essential to seek immediate medical attention if these symptoms occur.
3. Adhesions: Scar tissue may form after surgery, causing organs or tissues to stick together. This can lead to chronic pain, bowel obstruction, or other complications.
4. Nutritional deficiencies: After small bowel resection, absorption of nutrients may be affected. Your medical team will provide diet recommendations and may suggest supplements to prevent deficiencies and promote healing.
5. Diarrhea and malabsorption: Removal of a portion of the small intestine can result in changes in digestion and absorption, leading to diarrhea, malabsorption of nutrients, and weight loss. Dietary modifications and medication management may be necessary.
6. Fistula formation: Abnormal connections between different parts of the intestine or between the intestine and other organs may develop after surgery. These fistulas can cause infection, leakage of fluids or stool into other areas, and require surgical intervention.
7. Bleeding: Although rare, bleeding from blood vessels near the surgical site can occur during or after surgery and may require intervention.
Patients need to be aware of these potential complications and promptly report any concerning symptoms to their healthcare provider for appropriate management. Regular follow-up appointments with their healthcare team are crucial for ongoing monitoring and support post-surgery.
The Prognosis for Small Bowel Resection
The prognosis for small bowel resection is generally favorable, especially when the surgery is performed for benign conditions such as strictures or adhesions. Most patients can expect to regain normal bowel function and resume their regular activities within a few weeks or months after surgery.
However, the long-term outlook may be less favorable for patients who undergo small bowel resection for more serious conditions such as Crohn’s disease or cancer. In these cases, the prognosis depends on the extent of the disease and the effectiveness of any additional treatments, such as medication or chemotherapy.
Patients need to work closely with their healthcare team to develop a personalized treatment plan and to have realistic expectations for their long-term recovery.
A Note from Southlake General Surgery about Small Bowel Resection
At Southlake General Surgery, we understand the importance of providing comprehensive care and support to patients undergoing small bowel resection. Our team of experienced surgeons and healthcare professionals is dedicated to ensuring that each patient receives the individualized care they need to achieve the best possible outcomes.
We work closely with patients to develop a personalized treatment plan that considers their specific condition, medical history, and goals for recovery. Throughout the entire process, we are committed to providing clear communication, compassionate care, and ongoing support to our patients and their families.
Appointment

For more information on Small Bowel Resection. You can contact our healthcare expert today at +1 (817) 748-0200. You can also make an online appointment with us.
Frequently Asked Questions
What are the potential complications of small bowel resection?
The potential complications of small bowel resection include transient malabsorption, short bowel syndrome (SBS), and the need for permanent maintenance nutrition treatment.
How does the length of small bowel resected impact post-operative outcomes?
The length of small bowel resected has an impact on post-operative outcomes. Resection of more than 25 cm of the small bowel and more than 50 cm of the total (small plus large) bowel is associated with a decreased likelihood of recurrence. However, larger resections (50, 75, 100 cm) do not show a decreased likelihood of recurrence. Therefore, more extensive resections within the range of 25 to 50 cm are recommended, while still considering intraoperative judgment in determining the amount of resection.
What are the common factors that affect recovery time after a small bowel resection?
The common factors that affect recovery time after a small bowel resection include the need for parenteral analgesia (persistent pain), intravenous fluids (persistent gut dysfunction), and bed rest (persistent lack of mobility).
How long does recovery typically take after a small bowel resection?
On average, a full recovery from small bowel resection surgery can take up to three months. However, the specific recovery time can vary depending on factors such as the individual’s health before surgery, the location and severity of the condition being treated, and any complications that may arise during the recovery process. It is best to consult with a healthcare provider for a more accurate estimation of the recovery time in each case.
Is there a difference in recovery time between laparoscopic and open small bowel resections?
Yes, there is a difference in recovery time between laparoscopic and open small bowel resections. The mean time of first flatus and time to restart oral intake after surgery was shorter in the laparoscopic group compared to the open group. Additionally, the length of hospital stay was 3 days shorter for laparoscopic patients.
Medically Reviewed By: Dr. Valeria Simone MD
Board-certified General Surgeon at Southlake General Surgery, Texas, USA.
Follow us on Facebook and YouTube.
References:
- Clatterbuck, B. (2023, April 17). Small Bowel Resection. StatPearls – NCBI Bookshelf. https://www.ncbi.nlm.nih.gov/books/NBK507896/
- “Small and Large Bowel Resection.” Crohn’s & Colitis Foundation, www.crohnscolitisfoundation.org/what-is-crohns-disease/treatment/surgery/small-large-bowel-resection.
- Laparoscopic Bowel Resection: Before Your Surgery. (n.d.). https://myhealth.alberta.ca/Health/aftercareinformation/pages/conditions.aspx?hwid=zc2036